Prostate Cancer: What Every Person Should Know
Prostate cancer is the most commonly diagnosed cancer in Australia. Each year, over 24,000 men are diagnosed, where most men are over the age of 50. Chances are, most people will know, or know someone who knows someone who has been diagnosed with prostate cancer.
Where Is The Prostate and What Does It Do?
The prostate is a small gland that sits deep inside the pelvis in men, underneath the bladder and in front of the bowel. The urethra, which is the tube that comes out from the bladder that urine and semen travel through, passes through the prostate. It uses testosterone to help produce some of the fluid that makes up semen. Normally, the prostate is approximately the size of a walnut in an adult male and will slowly grow larger over time.
Diagnosing Prostate Cancer Is Complex
Prostate Cancer is not a straightforward disease, nor are the treatment options clear cut. There is are many investigations and tests that are undertaken to obtain a full picture of the prostate cancer diagnosis, including the state and severity of the disease. This might include:
- PSA Test: a blood test which examines the amount of Prostate Specific Antigen, which is a protein made by the prostate. It is normal for PSA to rise small amounts and very slowly as people age, but if it starts to increase very quickly and by a large amount, this may be a sign that more investigation is needed.
- Digital Rectal Examination: a doctor can feel the prostate by inserting their gloved finger into the back passage. They are able to determine if the feel of the prostate is abnormal. This will indicate the need for further investigation.
- MRI: a scan that looks into whole body and can reveal if there is cancer in the prostate, where it is located and if there are other problems in other parts of the body.
- Biopsy: a small needle is inserted into the prostate through the perineum or rectum. Small samples of prostate tissue are removed and then tested in a laboratory to determine if cancer is present, and how extensive it is.
- CT scan: a scan that can reveal if cancer has spread to other parts of the body.
- Bone scan: a scan that can see if any cancer cells are present in bone.
- PSMA PET scan: a newer technology that can identify the location of prostate cancer and if cancer is present in other parts of the body. If present, cancer cells show up brighter on the scan.
Once Doctors have collated enough information, they will be able to determine:
- The size of the prostate
- The grade of the cancer: how fast it is growing and how aggressive it is
- If the cancer has spread to other parts of the body
All of these factors will help to determine which treatment options are available. Other factors that are taken into consideration include:
- Age
- General health / other health related conditions
- Previous surgeries and past treatment eg radiotherapy
- Weight
- Emotional health
- Current or future relationship plans
- Quality of life
- Treatment preferences
Making A Decision About Prostate Cancer Treatment Is Difficult
Once a diagnosis has been made and the severity of the cancer has been established, a decision needs to be made about how best to treat it. There are a number of different treatment options available for prostate cancer and the decision regarding which treatment to have is ultimately made by the person with prostate cancer, considering advice provided by their Urologist, Oncologist, GP, Prostate Cancer Nurse and other trusted health professionals. It can also be helpful to get a second opinion.
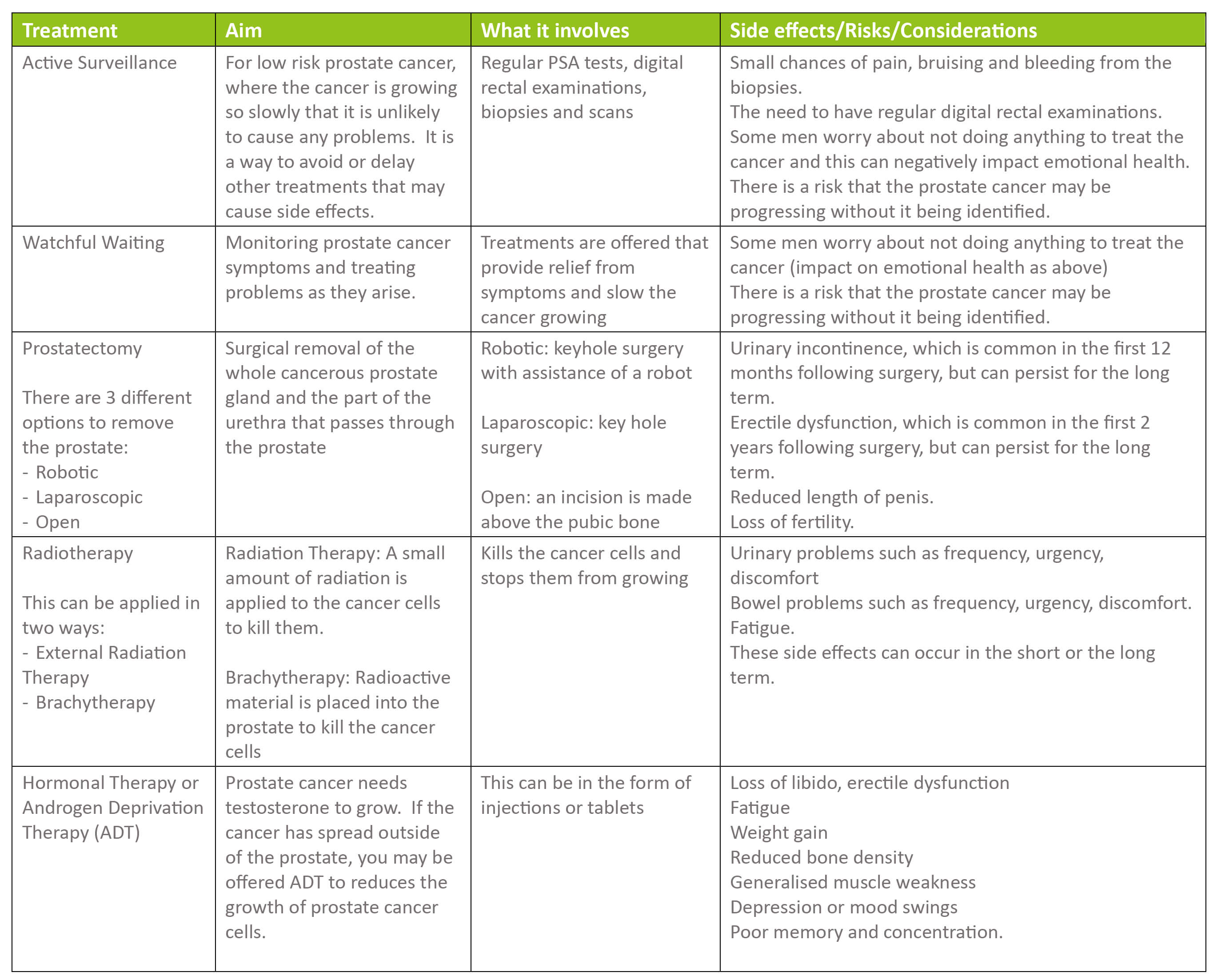
As you can see from the table below, the treatments of prostate cancer all come with significant side effects that have the potential to impact quality of life. The different options for prostate cancer treatment include:
Talk to your doctor, nurse, GP to ensure that you are fully informed and understand all of the treatment options available before making a decision. If you need help with your emotional health during this time, there is support available. Talk to your health care team, or call the Prostate Cancer Foundation of Australia on 1800 22 00 99.
Every Prostate Cancer Journey Is Different
Given that there is so many factors that determine the severity of the cancer, there are a number of treatment options available where the side effects of each treatment also vary, every person’s journey with prostate cancer is different.
When faced with a prostate cancer diagnosis, it can be reassuring to talk to other people that have also been diagnosed with prostate cancer. However, one person’s experience can be very different from the next person. For men that choose to undergo surgery to remove the prostate, the degree of incontinence experienced can vary greatly. Some men drip from time to time with changes in position, others spurt urine loss when they lift or swing a golf club, whilst other men feel a b like a leaky tap that won’t turn off. The degree of leakage is impacted by many factors; the degree and position of the prostate cancer, how much impairment to the bladder sphincter muscles occurs during surgery, age, weight, activity levels and other factors.
Survivorship For Prostate Cancer
In 2021, a group of Australian based Urologists, Psychologists and specialists in Prostate Cancer developed the Prostate Cancer Survivorship Essentials Framework. This was in response to evidence that showed for many men, they had unmet needs in relation to their emotional health. To read more about this, see our blog article “The Emotional Burden Of Prostate Cancer”
The group developed a plan that includes intervention options and support for survivors of prostate cancer. They acknowledge that any person who has had a cancer diagnosis is considered to be a survivor. Survivorship care means having a plan to look after your wellbeing now and for any changes that might happen in the future.
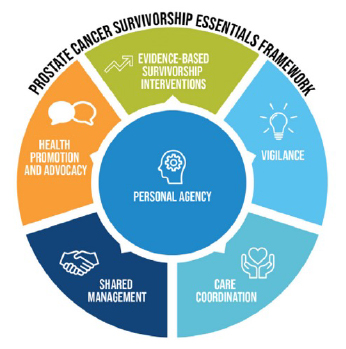
The plan includes 6 areas to consider, which includes:
- Personal Agency: understanding what support is available to you, what you need to do to help yourself and what others can offer you.
- Shared Management: being involved in decision making with your health care
- Vigilance: your health care team keeping on top of the control of the cancer, the management of side effects and also checking in on your emotional and social wellbeing.
- Evidence-based survivorship interventions: ensuring that your treatment and management is based on up to date research and evidence
- Care Coordination: your health care team communicating and working together to give you the best care
- Heath Promotion and Advocacy: having the most up to date and accurate information provided to you
This survivorship framework has been developed into a Wellness Plan, that can be used to summarise the information about diagnosis, treatment and progress. This plan can be downloaded from the Prostate Cancer Foundation of Australia
It Takes A Team Of People To Treat Prostate Cancer
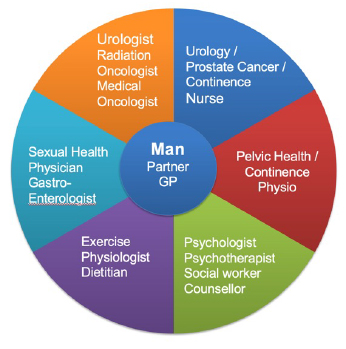
There are a number of people involved in the treatment of prostate cancer and it is important that your team work together and with you to help you through your cancer treatment journey. Some of the common specialists you might deal with are:
Writing down questions to ask your health care team can help to get the information that you need. Informing each member of your health care team who is in your health care team can help them to communicate about your progress and treatment.
You are your biggest advocate. Educate yourself, seek a second opinion and get your health care team communicating with each other to help you achieve the best outcome.
The Role Of Physiotherapy In Prostate Cancer
Pelvic Health Physiotherapy is recommended to everyone undergoing surgery for prostate cancer both before, and after their surgery. It is also recommended for those experiencing bladder or bowel side effects during/following radiotherapy.
To learn more about the role of physiotherapy on incontinence, read Greg’s story.
Read our article to learn more about Erectile dysfunction following prostate cancer treatment
At WMHP, all of our physiotherapists are highly experienced and post-graduate trained Pelvic Health Physiotherapists. We have led the way in the physiotherapy management of prostate cancer problems for other 30 years. We are proud to be able to support men and their partners through this difficult journey.
September, 2023